NEWS
NEWS
Turning one immune cell into another
- Scientists at the Centre for Genomic Regulation in Barcelona describe how a single molecule is able to turn an immune cell type into another
- The findings appear in the July 30 issue of the Stem Cell Reports journal and give new clues on induced transdifferentiation, which could become therapeutically relevant in the future.
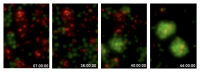
All it takes is one molecule to reprogram an antibody-producing B cell into a scavenging macrophage. This transformation is possible, new evidence shows, because the molecule (C/EBPa, a transcription factor) “short-circuits” the cells so that they re-express genes reserved for macrophage development. The findings appear July 30 in Stem Cell Reports, the journal of the International Society for Stem Cell Research.
Over the past 28 years, researchers have shown that a number of specialized cell types can be forcibly converted into another, but the science of how this change takes place is still emerging. Such transdifferentiations, as they’re called, include turning a skin cell into a muscle cell (or a muscle cell into a brown fat cell) with the addition of just one or two transcription factors. These are molecules that bind to a cell’s DNA and cause other genes to be expressed.
“For a long time it was unclear whether forcing cell fate decisions by expressing transcription factors in the wrong cell type could teach us something about what happens normally during physiological differentiation,” says senior study author Thomas Graf, group leader at the Centre for Genomic Regulation in Spain. “What we have now found is that the two processes are actually surprisingly similar.”
Based on experiments led by the first author of the study, Chris van Oevelen, B cell transdifferentiation takes place when C/EBPa binds to two regions of DNA that act as gene expression enhancers. Whereas one of these regions is normally active in immune cells, the other is only turned on when macrophage precursors are ready to differentiate. This indicates that the convergence of these two enhancer pathways can cause the B cell to act like a macrophage precursor, thus triggering the unnatural transdifferentiation.
“This has taught us a great deal about how a transcription factor can activate a new gene expression program (in our case, that of macrophages) but has left us in the dark about the other part of the equation; namely, how the factor silences the B cell program, something that must happen if transdifferentiation is to work,” Graf says. “This is one of the questions we are focusing on now.”
Graf is interested in this pathway because C/EBPa-induced, B cell-to-macrophage transdifferentiation can convert both human B cell lymphoma or leukaemia cells into functional, non-cancerous macrophages. He believes that induced transdifferentiation could become therapeutically relevant, if a drug could be found that can replace the transcription factor—not to mention that understanding the mechanisms of the process would help labs worldwide who use this transdifferentiation approach to generate cells ”a la carte” for regenerative purposes.
************************************
This work was primarily supported by the Ministerio de Educacion y Ciencia, the EU-FP7 project BLUEPRINT, and the Fundacio la Marato. Additional funding was received from Leukemia Lymphoma Research UK.
Reference: Stem Cell Reports, van Oevelen et al.: “C/EBPα activates pre-existing and de novo macrophage enhancers during induced pre-B cell transdifferentiation and myeloid lineage specification” http://dx.doi.org/10.1016/j.stemcr.2015.06.007
Media Contact: Laia Cendrós – Press Officer – Centre for Genomic Regulation (CRG) - Ph. +34 93 316 02 37.
| Attachment | Size |
|---|---|
| 119.63 KB | |
| 121.74 KB | |
| 120.26 KB |